We offer numerous general and advanced surgical services, right here in Sampson County. Below, you will find descriptions of what surgeries we offer and information on what the procedures entail.
Caring Hands Animal Hospital is equipped with a sterile surgical suite, regularly maintained anesthesia machines, and a full array of state-of-the-art surgical and monitoring equipment
Our skilled doctors can perform many surgeries in-house, allowing for continuity of care for elective procedures, and minimizing transfer time in emergency situations. In some cases a pre-surgical consult will be scheduled to discuss risks, benefits, recovery, and any other concerns you may have regarding your pet's surgical procedure.
Our surgical capabilities and level of care strongly correlate to healthy pet, happy life!
Soft Tissue Surgeries
- Spay (ovariohysterectomy)
- Neuter (castration)
- Prophylactic gastropexy/GDV (gastric dilation and volvulus)
- Hernia (Traumatic/Non-Traumatic)
- Oncologic surgery (tumor removal-external/internal/lumpectomy)
- Gastric/Intestinal repair, foreign body removal/resection and anastomosis.
- Splenectomy
- Ocular/Eyelid repair (entropion, cherry eye repair, enucleation)
- Urologic surgeries (cystotomy, urethrotomy, perianal urethrostomy)
- Caesarian Sections (C-Sections)
- And many more!
Orthopedic Surgeries
- Fracture repair (Plating, plate/rod, cross pin, compressive screw, etc.)
- Femoral Head Osteotomy (FHO)
- Amputations
Fracture Repair Services



At Caring Hands, while our doctors are general surgeons and not board-certified orthopedists/surgeons, they are orthopedically trained by the AO organization which is a prestigious international orthopedic foundation that focuses on orthopedic care in both human and veterinary patients. We offer robust fracture repair options through the use of high-quality plating systems, rods, pins, wires, and screws. If you're worried that your furry loved one has broken his/her leg, our doctors will start by taking x-rays and then will develop a plan using special fracture planning software before operating. We will provide you an honest estimate, and provide you with several options of how to carry that plan out which in limited situations may include referral to specialists if its a case we don't feel comfortable operating on. We do take referrals from other hospitals that don't operate on bones! Give us a call and we will happy to serve you in anyway we can.
Caring Hands is proud to use very high quality human-quality orthopedic plating equipment (Movora/VOI) and orthopedic drills (Stryker)


- bending (like the force used to break a pencil in half)
- torsion (a twisting force around the bone)
- compression (the force that gravity puts on us when we bear weight on our legs)
- traction (the pulling force applied to a small portion of bone by a muscle at its attachment on the bone)
The strength of normal, healthy bone resists these forces. A bone breaks when it is subjected to a force that is greater than its own strength. Once it is broken, it must be immobilized sufficiently to allow the bone to heal back together. This is where veterinary treatments, like those listed below, are used to ensure quality bone healing and good leg use.
External coaptation: a splint or cast; applied to the outside of the limb; good at resisting bending forces and fair at resisting torsion and compression forces.
Internal fixation: surgically applied devices implanted inside the bone or on the surface of the bone. Various devices are available and offer different results against the various forces such as plates, screws, nails, pins, wires.
Several factors go into making up a final treatment plan for a fracture. Each factor has characteristics that support easy/rapid fracture healing and characteristics that result in slow/complicated fracture healing. We use this scale of information to come up with the best repair options for an individual pet.
-American College of Veterinary Surgeons
FHO/FHNE

An FHO, or femoral head ostectomy, is a surgical procedure that aims to restore mobility to a damaged hip joint. By removing or excising the ball portion of the hip joint and smoothing the bone so there is no bone to bone contact occurring between the pelvis and the remaining portion of the femur, thus eliminating a majority of pain and discomfort in your pet.
When the hip becomes damaged or diseased, mobility can be affected. If the ball joint of the hip and the head of the femur do not fit together properly, the degree of movement that the joint can achieve is lessened. In addition, this poor joint fit can lead to chronic pain and inflammation.
An FHO restores mobility to the hip by removing the head of the femur. This removes the ball of the ball-and-socket joint, leaving just an empty socket. The muscles of the leg will initially hold the femur in place and, over time, scar tissue will form between the joint of the hip or acetabulum and the femur to provide cushioning that is referred to as a 'false joint'. Although this joint is anatomically very different from a normal hip joint, it provides pain-free mobility in most patients.
The primary goal of an FHO is to remove bone-on-bone contact, restoring pain-free mobility. The most common reasons for FHO include:
- Fractures involving the hip. When a fracture involves the hip joint and cannot be repaired surgically an FHO may provide the best option for pain-free mobility.
- Hip luxation/dislocation (associated with trauma or severe hip dysplasia). In some cases, a hip that is out of socket cannot be replaced with manipulation or other medical means. Surgical repair of hip luxations can be costly and is not always successful, so many dog owners elect FHO for small dogs with hip luxation.
- Severe arthritis of the hip. In chronic, end-stage arthritis, the cartilage that protects both the head of the femur and the acetabulum can become eroded away, leading to painful bone-on-bone grating whenever the hip is moved. Performing an FHO can remove this point of contact and alleviate pain.
- Legg-Perthes disease. This uncommon condition, most frequently seen in miniature and toy breed dogs, causes the bone within the femoral head to begin to die at an early age. The bone collapses due to these degenerative changes, leading to severe pain. Removing the femoral head via FHO removes the source of pain for the dog.
Hospitalization of patients for FHO surgery typically ranges from 2-3 days including the day of the surgery and recovery. In general, most patients are discharged 1-2 days after their surgical procedure.
Most dogs recover fully after FHO surgery and regain essentially-normal function of the affected leg. Although the leg may have a slightly decreased range of motion or decreased limb length after surgery, these impacts are typically minimal and do not impact the pet’s quality of life.
Gastropexy
Gastropexy (commonly known as a “pexy” or “tacked stomach”) is an elective surgery which involves permanently adhering one end of the stomach to the body wall. This procedure is the most effective way to prevent Gastric Dilation and Volvulus (GDV), which is a complication of Bloat. It is often performed at the time of spay or neuter, while a dog is already under anesthesia, and is recommended for many large and giant breed dogs, particularly those dogs who are considered to be deep-chested.
Breeds for which gastropexy is commonly recommended:
- Great Dane
- Golden Retriever
- Labrador Retriever
- German Shepherd
- Setter breeds
- St. Bernard
- Weimaraner
- Boxers (depending on size)
- German Short Haired Pointers (depending on size)
- Standard Poodle/Doodle breeds
What is Bloat and GDV?
Bloat is when the stomach becomes filled and distended with air, GDV is a complication which occurs when the air-filled stomach twists on itself, compromising blood flow to the stomach tissue.
Factors that increase the risk of bloat:
- Family history
- Being thin or underweight
- Feeding only 1 meal per day
- Eating rapidly
- Feeding from an elevated bowl
- Restricting access to water
- Diets with fat in the first 4 ingredients
- Fearful or anxious temperament
- Males are more likely to bloat than females
- Bloat occurs more commonly in dogs over age 7
Contrary to popular belief, cereal ingredients such as soy, wheat, or corn in the first four ingredients of the ingredient list do not increase the risk of bloat
Factors that decrease risk of bloat:
- Including canned food in the diet
- Eating 2 or more meals per day
- Feeding a dry food containing a calcium-rich meat meal (such as meat/lamb meal, fish meal, chicken by-product meal, or bone meal) listed in the first four ingredients of the ingredient list Signs of Bloat Signs of bloating and GDV include heavy panting, painful stomach, distended abdomen, and nonproductive retching, although dogs may bloat without developing these specific symptoms.
If a dog does bloat, they require emergency treatment by a veterinarian. Without treatment, most bloated dogs will die within a matter of hours (if they have not previously received a gastropexy).
Why Gastropexy?
Even though most dogs will not bloat in their lifetime, for those who do suffer from GDV the morbidity and mortality rate is extremely high. In patients who have already received a gastropexy, the stomach can usually be safely decompressed and the patient stabilized quickly. Dogs who have not had a gastropexy often require emergency surgery to correct the torsion of the stomach and a gastropexy to prevent a recurrence. In many dogs with GDV sections of the stomach, tissue have died from lack of blood flow and must be removed, which increases the likelihood of post-surgical complications. Without gastropexy, up to 75% of these dogs will bloat again in their lifetime.
The most effective way to prevent GDV is to have your dog receive a gastropexy at the time of spay or neuter. Gastropexy can also be performed at any time on an adult dog. If you think your pet is a candidate for gastropexy please schedule an appointment with your veterinarian, we will be happy to discuss your pet’s individual needs.
Splenectomy
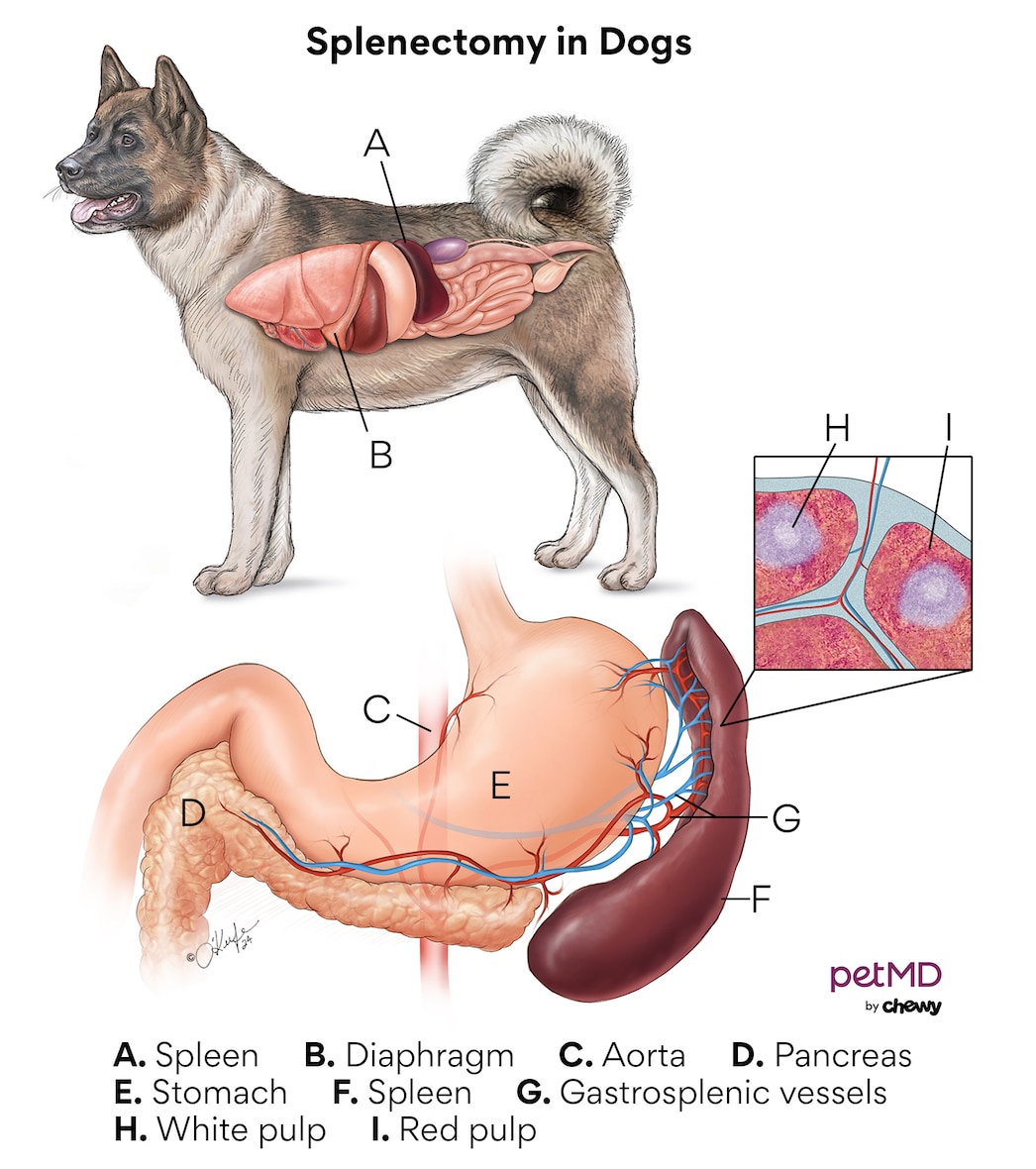
Splenectomy is a procedure to remove the spleen. Most commonly, a complete splenectomy is performed. A full open abdominal exploratory surgery is typically performed, allowing for access to the full blood supply and for evaluation of other abdominal organs. Removal of the spleen can serve as a diagnostic and therapeutic endeavor. During surgical exploratory, biopsy of other organs (such as liver or lymph node) may be performed. Prior to surgery, bloodwork, blood pressure monitoring, EKG monitoring, x-rays or an abdominal ultrasound may be recommended.
A majority of patients undergoing splenectomy on an emergency basis have hemorrhage from the spleen. Prior to surgery, these patients are often stabilized with fluid support and blood products or intensive care monitoring, as necessary. Upon removal, the spleen is often sent to a pathology lab for biopsy (histopathology) to obtain a definitive diagnosis.
Cystotomy

A cystotomy is when a surgeon cuts into the bladder to remove either stones, sludge, crystals, or sometimes tumors to prevent blockages or irritation in the bladder.
What are Bladder Stones?
Bladder stones are literal stones that form from pH and crystal formation problems within the dog/cat's body. Overtime the stone precursors (i.e. crystals) clump together and form stones. These stones bounce around in the bladder and irritate the bladder and can also hold bacteria leading to chronic UTIs. Some stones can be dissolve by special diets, but some stones require surgical removal. Some stones can grow to the point of causing an obstruction. Both partial and full obstructions are possible.
Clinical signs depend on the severity of the blockage. Dogs that have a partial obstruction may:
- urinate small amounts frequently
- take a long time urinating
- strain to urinate
- have blood in the urine
- urinate in drips instead of a strong stream
- urinate in inappropriate places (on the carpet or on their bedding)
If the urethra is completely blocked, your dog/cat will strain without producing any urine. He/she will be in pain and be lethargic, lose their appetite, and possibly start vomiting. An overly large urinary bladder will be easily felt in the back half of the belly. (Caution: it may be painful when touched). The urinary bladder may rupture and spill urine into the patient's abdomen with complete obstruction. Patients with total urethral obstruction will die within days if the obstruction is not relieved. Your pet should be seen by a veterinarian immediately if he/she is unable to urinate.
Urinary tract calculi are the most common cause of urethral obstruction in dogs and cats, anything that causes stone formation will increase the risk of urethral blockage (see urinary stones). For example, Yorkshire Terriers and Schnauzers with liver shunts (see portosystemic shunts) and Dalmatian dogs are prone to forming urate calculi. Kidney, bladder, and prostate infections can increase the risk of struvite calculi formation.
What is a Cystotomy?
If the obstruction is caused by urinary tract calculi, your veterinarian will try to flush the stones back into the bladder, where they can either be removed surgically, dissolved with medical management (depending on the type), or broken up with lithotripsy (smashing of stones with ultrasonic waves or lasers). If your dog/cat is very sick, surgery may be delayed, and a urinary catheter left in the urinary tract to drain urine from the bladder for a day or two, until medical conditions have improved and your pet is stable for general anesthesia and surgery.
To remove stones from the bladder surgically, a cystotomy procedure is performed. In this procedure, the patient is under general anesthesia. The bladder is accessed through a small abdominal incision. Then the bladder is opened, stones are removed, and the urinary tract is flushed thoroughly to make sure no stones are left behind. If stones in the urethra cannot be flushed into the bladder for removal, a separate incision into the urethra may be necessary. Stones removed at surgery are submitted for chemical analysis and in some cases, for culture as well. Biopsy of any abnormal bladder tissue may be collected as well.
Patients which have a urethral obstruction that cannot be unblocked, have a tumor of the penis, or are recurrent stone formers may require surgery to form a new permanent opening to the urethra, called a scrotal/perianal (for cats) urethrostomy. Urethrostomies may be required because calculi in the urethra may become trapped in scar tissue and therefore cannot be removed. A scrotal urethrostomy allows urine to exit behind the os penis where the urethra is wider. An opening is created that small stones may pass through. Patients with a scrotal urethrostomy may still get urinary obstruction by very large stones in the bladder or upper urethra. For most dogs having a scrotal urethrostomy, the penis is left in place, so your male dog will look the same when he is walking down the street. However, he will urinate from the new opening in the location where his scrotum used to be. In dogs with penile tumors, a scrotal urethrostomy is performed and the penis is removed. Because the surgery site is in the area of the scrotum, dogs are castrated (aka neutered) during the procedure.
-American College of Veterinary Surgeons
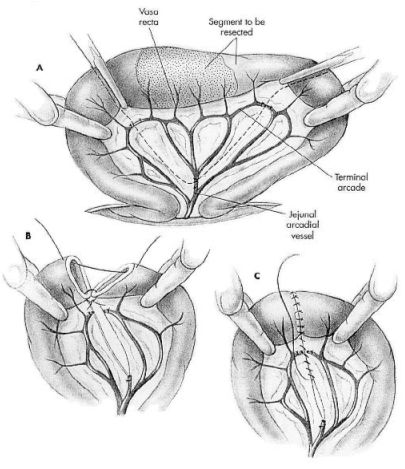
Enterotomy/Resection and Anastomosis
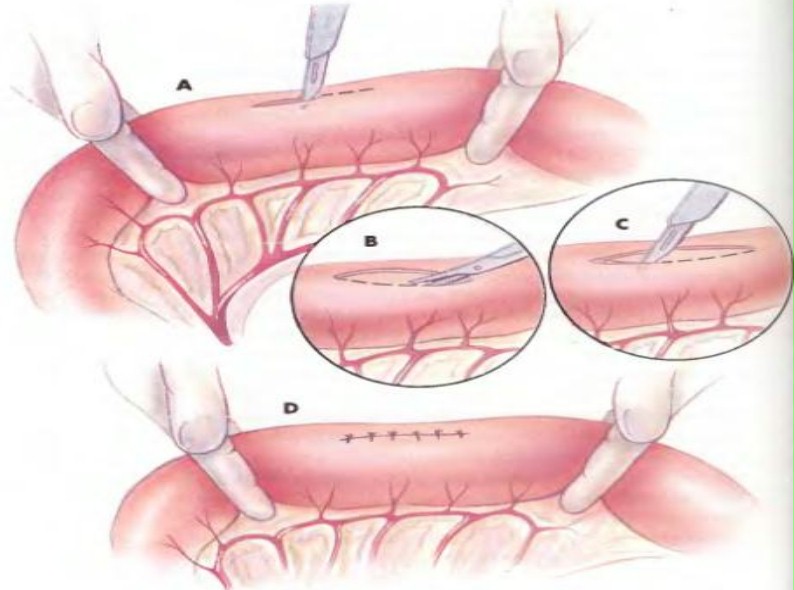
Gastrointestinal (GI) foreign bodies occur when pets consume items that are non-digestible and will not readily pass through their stomach or intestines. These items may be toys, leashes, clothing, sticks or any other item that fails to pass, including human food products such as bones or trash. When these items become lodged in the GI tract, they can cause the animal to become very sick. The problems that are caused vary with:
- how long the foreign body has been present.
- the location of the foreign body.
- how badly the foreign material closes off the opening of the GI tract.
- what the material is made of. Some ingested items, such as older pennies or lead material, can cause systemic toxicities while others may cause regional damage to the intestinal tract itself due to compression or obstruction.
Clinical signs can vary significantly with the degree of obstruction, location, duration, and type of foreign body. Commonly noted signs include:
- vomiting
- anorexia (loss of appetite)
- abdominal pain
- dehydration
- diarrhea (with or without presence of blood)
In cases of linear foreign bodies, a string may be observed wrapped around the base of the tongue (Figure 1) or coming out of the anus.
The symptoms of a foreign body or intestinal obstruction can cause dehydration and electrolyte imbalances. This can cause the pet to feel systemically ill as well. Additionally, if the foreign body has perforated the GI tract and entered the chest or abdominal cavities, the animal may be profoundly ill and in critical condition. These may cause peritonitis, sepsis, and death. Many foreign bodies are made of materials that are potentially toxic when absorbed. Lead and zinc are good examples that when consumed may lead to profound systemic disease if enough is absorbed.
Gastrointestinal foreign bodies, especially strings, can sometimes cause holes in the tissue (or perforation). This causes spillage of intestinal contents into the abdomen. This condition quickly leads to life-threatening inflammation of the abdominal lining (peritonitis) and allows bacterial proliferation and contamination (sepsis). While some small foreign bodies will pass, many will become lodged along the gastrointestinal tract and cause discomfort and make your pet sick. Some foreign bodies located in the stomach may be retrieved with the use of an endoscope; however, most require surgical abdominal exploration and removal. Occasionally, foreign bodies will become lodged in the esophagus at the base of the heart or at the diaphragm, which may require thoracic (chest) surgery.
Your primary care veterinarian will likely recommend initial blood work that includes a complete blood count (CBC), serum chemistry, and a urinalysis. These combined will help to rule out other causes for your pet’s symptoms. Abdominal, and occasionally thoracic, radiographs are regularly performed (Figures 2 and 3). Positive contrast radiographs (using barium to highlight the inside of the stomach and intestines) may be performed when routine radiographs fail to show the cause for the clinical signs. Abdominal ultrasound can be very helpful in identifying gastrointestinal foreign bodies.
Surgery is not always required with gastrointestinal foreign bodies. Occasionally, the item ingested is small and smooth enough to pass through the gastrointestinal tract without causing damage or becoming lodged. Your veterinarian may recommend hospitalization for intravenous fluids and monitoring to help the item pass in this case. Additionally, some foreign bodies may become lodged in the upper gastrointestinal tract (mouth, esophagus, and stomach) and may be retrieved by making the pet vomit or with the use of a flexible endoscope (tube with a camera). If conservative management and endoscopy fail to provide relief, if the foreign body is not moving on x-rays, if the obstruction is getting worse, or if there is evidence of a linear foreign body, surgical exploration is warranted.
Esophageal foreign bodies require thoracic (chest) surgery to gain access for removal. Most gastrointestinal foreign bodies become lodged within the stomach or intestines and require a gastrotomy (opening the stomach) or enterotomy (opening the intestine). Once the item has been removed, the gastrointestinal tract is closed. Many linear foreign bodies and completely obstructed intestines are damaged severely enough that multiple enterotomies may need to be performed. If a section of bowel is irreversibly damaged, the section is removed and the healthy ends are reattached (an intestinal resection and anastomosis). The decision of which procedure to perform is determined by the surgeon when all the intestines and other abdominal organs have been evaluated.
-American College of Veterinary Surgeons
Pyometra
Pyometra is an infection of the uterus that may occur in dogs and cats making the pet very ill. The uterus is generally filled with pus. Although the disease has been recognized for decades, the true disease process has still not been completely understood. It is generally recognized that progesterone and estrogen and their receptors have a role in the development of pyometra; however, the infection is triggered by bacterial involvement.
The cyclical hormonal influences of the female dog and cat allow the uterus to go through changes that will be acceptable for fertilization of an embryo. If bacteria are introduced into the uterus at a certain time during the cycle, hormonal regulation of the uterus allows the infection to start and become life-threatening. The bacteria typically cultured from the uterus are bacteria that would be found in the areas of the intestines and vagina (E. coli is the most common). Therefore, many of the infections are considered either from an ascending infection from the vagina, a concurrent urinary tract infection, or fecal contamination.
Most dogs and cats that are spayed early in life will not develop pyometra. However, a uterine stump pyometra may occur after incomplete ovariohysterectomy which allows a segment of the uterine body or horn to become infected. Typically, either a portion of the ovarian tissue is still present or the animal has been subjected to pregestational hormones to allow this situation to develop.
Because the infection can be so severe, the signs your pet may show are not limited to the genital tract. Your pet can become so overwhelmed by the inflammation associated with the infection that the uncontrolled inflammatory process may be life-threatening.
The most common clinical signs in dogs and cats are:
- lethargy
- depression
- anorexia
- excessive water intake
- excessive urination
- pale mucous membranes
- bloody vaginal discharge
Vomiting, diarrhea, weight loss, abdominal distension, and inflamed eyes have been reported less frequently. Some pets may have no clinical signs other than purulent vaginal discharge. Pyometra should be considered in any intact female dog that is sick.
Many dogs and cats will have a closed cervix and therefore the obvious sign of bloody vaginal discharge may not be present.
Your primary-care veterinarian may suspect the diagnosis based on your history and your pet’s physical exam. If the cervix is not open, the diagnosis may take a few more diagnostic tests. In general, a fluid distended uterus is needed to diagnose pyometra. Your veterinarian will likely recommend the following diagnostic tests to help diagnose pyometra:
- general chemistry profile
- complete blood count
- urinalysis
- abdominal radiographs
- abdominal ultrasound
- vaginal cytology
Radiographs are typically very suggestive but abdominal ultrasounds will typically identify the fluid filled uterus
Pyometra is a medical emergency that requires rapid intervention to prevent overwhelming infection and death. For most pets, preoperative stabilization and resuscitation are first and foremost. After appropriate stabilization, ovariohysterectomy (spay) is the therapy of choice. The results of this therapy are generally a rapid recovery with minimal risk of recurrence. Ovariohysterectomy also negates the risk of ovarian and uterine cancer and future unwanted pregnancy.
Although surgery is the therapy of choice, very special case selection meeting certain criteria may allow valuable breeding animals to be treated medically. However, in addition to the previously mentioned multiple organ problems, the dogs will generally exhibit abdominal pain, excessive vomiting/ defecation, high heart rates, salivation, breathing difficulties, panting, and fever with medical management. It takes several days until an effect is seen when treating pets with pyometra with injectable prostaglandins and antibiotics. Dogs and cats are susceptible to developing pyometra again after medical treatment and should have an ovariohysterectomy performed when their breeding purposes are finished.
-American College of Veterinary Surgeons
Enucleations
There are several conditions of the eyes, which can be painful or blinding. Although the goal of a veterinary ophthalmologist is to try to save eyes and vision, wherever possible, sometimes removal of an eye (enucleation) is necessary. Some possible reasons for removal of an eye include uncontrolled glaucoma (increased intraocular pressure), a tumor inside the eye, or severe trauma to the eye. Although this can seem like a drastic option, enucleation is a relatively common procedure.
If you have been referred to a veterinary ophthalmologist for evaluation, they will first examine your pet to determine what may be going on. If your pet is diagnosed with a vision threatening or painful condition, treatments options may be available to try to preserve the eye. Alternatively, you may have been referred to a veterinary ophthalmologist to discuss enucleation. If it is determined that there are not viable treatments available, then enucleation may be recommended. Enucleation can resolve a painful condition and the eye can be submitted to a pathologist for evaluation, which can have prognostic value.
As mentioned above, an enucleation is the removal of the eye itself, as well as the upper and lower eyelids and the 3rd eyelid (also called the nictitating membrane). Your pet will be anesthetized, the fur clipped from around the eye and the eye will be surgically removed. The orbit (bony surrounding socket of the eye) can be left empty or a silicone orbital prosthesis may be placed. An orbital prosthesis is not recommended for cases with concern about infection or cancer. The remaining eyelid skin will then be carefully stitched closed. After surgery, there may be some swelling and bruising of the surgical site, but this will resolve with time. Your pet will go home with an Elizabethan collar, to protect the surgical site while it heals. The skin sutures are usually removed 10-14 days after surgery. If an orbital prosthesis was not used, over time, the area of eye removal may look sunken, although this is not an issue for your pet!
Since an enucleation is typically performed in blind or painful eyes, most pet owners find that their pets tolerate removal of the eye very well and are back to acting normally in a matter of days. In fact, removal of the eye can actually improve your pet’s quality of life.
In some cases, there may be alternative options to enucleation, such as an intrascleral prosthesis (an implant inside the eye itself) or an intravitreal injection (medication injected inside the eye to control glaucoma). For more information please talk to your veterinarian or find a veterinary ophthalmologist near you.
-American College of Veterinary Ophthalmologist
Entropion
What is Entropion?
Entropion is an ocular condition frequently identified in most companion animals. It is a rolling-in of the eyelids, and can involve the upper or lower eyelids, and in some cases, both. It can be unilateral (only one eye involved) or bilateral (both eyes involved). Entropion causes discomfort due to the hair and/or lashes rubbing on the cornea. Corneal ulcerations, perforations, and scarring can occur.
What causes Entropion?
In most of cases seen in dogs and cats, the cause is breed-related, or genetic in etiology. Several breeds of dogs have an increased incidence of entropion, including Chinese Shar Pei’s, Chow, Chows, Labradors. Entropion is also seen commonly in Maine Coon Cats. Breed-related entropion is caused by a conformation abnormality of the eyelid, causing contraction of the eyelid muscle and rolling in. The exact mode of inheritance of entropion is not known at this time.
Spastic entropion can be associated with ocular discomfort, causing contraction and rolling-in due to pain from corneal ulcers, foreign bodies, etc. Spastic entropion can often be differentiated from conformational entropion through the application of topical anesthetics. When the discomfort is alleviated, the lid relaxes.
Entropion is also seen secondary to inflammatory or age-related changes that cause enophthalmos. Enophthalmos occurs when the globe sits further back in the orbit than normally. This allows the lids to roll in toward the globe.
Cicatricial entropion is seen less commonly and is due to scarring of the eyelids or conjunctiva, causing contraction of the eye lids toward the globe.
How is Entropion diagnosed?
Entropion is usually easily diagnosed through a thorough ocular examination when chronic discomfort, inflammation, or ulceration is observed.
How is entropion treated?
In young animals, temporary tacking of the eyelids may allow the animal to “outgrow” the entropion as the anatomy of the head matures. The tacking decreases the discomfort and resulting spastic component. Prior to surgical correction, the health of the cornea, and increased comfort can be obtained with the use of lubricants.
Most entropions are surgically corrected. Several successful surgical techniques are employed, the most common of which is the modified Hotz-Celsus procedure.
Recently, collagen or Hyaluronic acid compounds have been used as fillers to “puff out” the entropic eyelids in elderly animals that are poor candidate for surgical correction.
What is the prognosis for Entropion?
If left untreated, entropion can lead to vision deficits caused by corneal ulceration, corneal perforation or severe scarring.
With proper diagnosis and treatment, the prognosis is excellent for maintain comfort and a healthy, visual eye.
--American College of Veterinary Ophthalmologist
"Cherry Eye" (Prolapsed 3rd eyelid)
“Cherry eye” is another way of saying that there is a prolapsed (stuck out) gland of the third eyelid. This prolapsed gland is the main tear producing gland for the eye, and produces between 40—60% of the tear film. When the gland becomes prolapsed, the ductules that normally release the aqueous (watery) part of the tear film become bent in half like a kinked garden hose, and the gland becomes chronically exposed to air. This often allows the gland to take on a swollen, congested, and very red appearance, which is how this condition has earned the name "cherry eye." Although the underlying cause for this condition is not completely understood, there appears to be a definite genetic component in several breeds, including the English Bulldog, Beagle, American Cocker Spaniel, Lhasa Apso, Pekingese, Mastiff, Poodle, any brachycephalic ('flat-faced') dog, and the Burmese cat. However, any dog or cat breed can be affected. Prolapse of the third eyelid gland can be unilateral or bilateral, and if both eyes are affected, they may not be affected at the same time. Most dogs affected by a third eyelid gland prolapse experience initial prolapse of the gland between 1—2 years of age.
It is believed that prolapse of the third eyelid gland occurs secondary to a congenital weakness of the anchoring tissues of the gland (meaning that affected animals are born with this abnormality, but that this abnormality may or may not be genetic). Once this connective tissue attachment has broken down, the connective tissue cannot be replaced. However, it is of critical importance for the health and comfort of the affected eye(s), as well as for the vision of the affected eye(s), to return a prolapsed gland to its normal anatomic location.
Ideally, a prolapsed gland should never be excised or removed, as this can immediately result in permanent dry eye (called keratoconjunctivitis sicca or KCS), as the third eyelid gland is the main tear producing gland of the eye. Additionally, standard tear stimulant medication that is used to treat dry eye almost always requires the presence of the third eyelid gland in order to work, and without the third eyelid gland in place to receive medications, secondary complications can lead to blindness in the affected eye(s), and even loss of the eye.
Surgical replacement of the prolapsed third eyelid gland is absolutely required in order to attempt to restore normal health to the third eyelid gland and secondarily to the eye. Several different surgical procedures can be used to replace a prolapsed third eyelid gland. The Morgan pocket imbrication technique is typically the surgical procedure of choice, as this procedure allows for the best return to normal anatomic function with least damage to the tear ductules. This procedure is sometimes combined with a third eyelid cartilage tacking technique (the intranictitans tack) for increased stability of the gland. Other procedures that tack or 'anchor' the gland to an extraocular muscle, the periosteum (bony membrane) of the orbital rim, or even the sclera (the outer shell of the eyeball itself) are ways to correct a prolapsed gland, but can restrict the mobility of the third eyelid gland, and can be somewhat more invasive. The ultimate choice of surgical repair method is decided upon by the surgeon at the time of surgery, when deep tissues can be thoroughly evaluated when your pet is relaxed and asleep.
Many (but not all) animals who have a prolapsed third eyelid gland may also have a concurrent third eyelid cartilage abnormality that may have predisposed or contributed to the prolapse of the gland, or may have been caused by the prolapse of the gland. If a cartilage deformity is left untreated, the risk of gland prolapse recurrence becomes greater than normal.
Additionally, many (but not all) animals who experience a prolapse of the third eyelid gland also have a condition known as macroblepharon, meaning that the length of the eyelids are abnormally excessive. Without proper tension between the eyelids and the eyeball, a previously prolapsed third eyelid gland is more likely to re-prolapse in the future. Therefore, if macroblepharon is noted prior to surgery, eyelid length should be corrected as a preventative measure for BOTH eyes. This does not change the appearance of the face, but often helps to eliminate issues of re-prolapse, and helps to improve long-term ocular health.
Following surgical replacement of a prolapsed third eyelid gland, there is FOREVER a risk for the development of dry eye. The risk for future development of dry eye is greatest in animals who have experienced CHRONIC prolapse of the gland prior to surgery, and in breeds that are otherwise genetically predisposed to the development of dry eye. Therefore, it is important that tear production is assessed in both eyes at least twice yearly by a veterinarian.
Success rate following surgical repair of a third eyelid gland prolapse with a veterinary ophthalmologist is approximately 92%, meaning that recurrence following surgery is less than 8%, and success is generally made even greater by proper post-operative recovery.
-American College of Veterinary Ophthalmologists